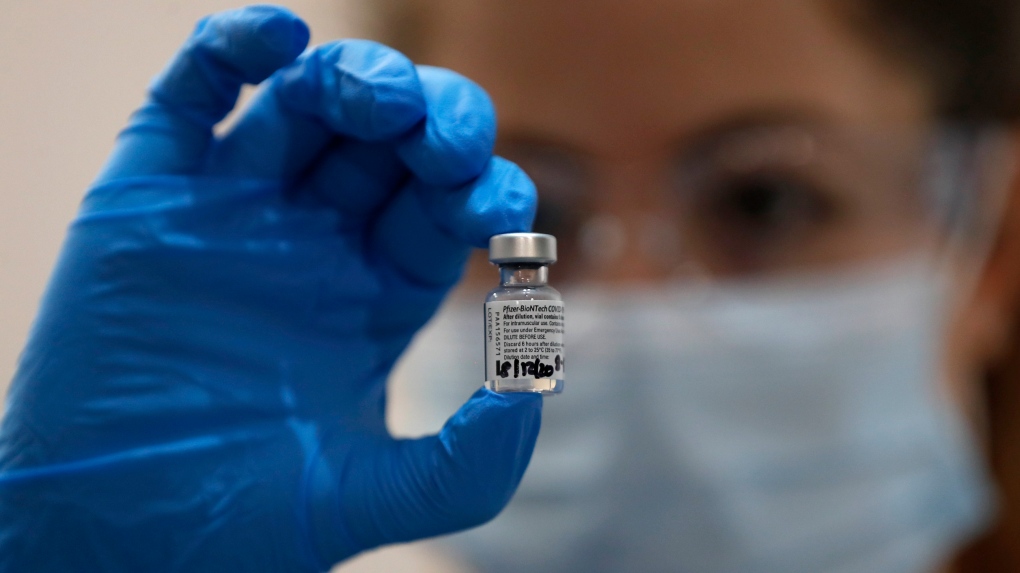
SASKATOON -- Saskatchewan is set to begin its rollout of Pfizer’s COVID-19 vaccine on Dec. 15, just under a year after the first cluster of novel coronavirus patients was reported in China. It’s the quickest any vaccine has been developed and Health Canada is also reviewing other candidates.
CTV News spoke with Volker Gerdts, director and CEO of VIDO-InterVac at the University of Saskatchewan, a lab dedicated to infectious disease and vaccine research, to learn about how these vaccines have been developed so fast, whether they present any new safety concerns, and the status of VIDO-InterVac’s own vaccine candidate. This interview has been edited for length and clarity.
How long does it usually take to develop a vaccine?
Normally, for human vaccines, it can take up to 10 to 12 years for a human vaccine. For animal vaccines it’s usually much faster, but even then it's still years before you have a product.
So how was this vaccine able to be completed in a tenth of the time?
Well, it's through a very concerted effort, through a lot of money and through the willingness to, along the production or the development pathway, lose money.
So if I can use just a very simple analogy: if you are willing to send 10 horses into the race, knowing that at the end, you only need one and you maybe lose nine, you can accomplish much more than running and then testing 10 different candidates in a sequence. Right? And so, this year, many governments around the world or big international organizations have made large amounts of money available to manufacturers to develop a vaccine as quickly as possible.
And so with that money, you're able to test multiple candidates, knowing that some of them may not work and others will. And if you are prepared to lose that money, you can obviously save some time by running them all in parallel.
And the other thing that people have done is trying to do as many activities in parallel as possible. So same idea, instead of waiting until you have the data from the first step to then go into the next study, processes have taken place in parallel. People were willing to, like I said, invest and lose money, but also, you know, try to reduce the time in between these studies to the bare minimum.
In general, how vaccines are typically made?
Okay, so in very simple terms, vaccines contain fragments, pieces if you want, of a pathogen in them. And those fragments, those pieces, are being produced in different systems.
So you can have that piece being a piece of RNA, as Pfizer or Moderna vaccines are, or you can make a protein as we do, or we can deliver it with another vector, another virus, which is the AstraZeneca vaccine.
Essentially, what you do is you take a part of the pathogen, you can also take the whole pathogen, but you make it non disease causing, and then you inject it and you show it to the immune system and the immune system recognizes it and forms an immune response to it.
We are trying to use a safe form of the pathogen. So often we kill these pathogens, we chemically inactivate them, so then they can’t cause disease anymore and then we can inject them. Or we just take fragments, pieces of those pathogens. And we pick the ones that are very important in the interaction between the pathogen and the host.
For example, right now, with the COVID-19 pandemic, everybody is focusing on this spike protein, which is on the surface of the virus, and that's what the virus uses to attach to the cells.
If you have an immune response against the spike protein, you have antibodies in your blood, they prevent the attachment of the virus to the host cell, and that's how we prevent the virus from causing disease.
I also understand that production of some of the candidates had started even before there was final approval just to get them out the door faster when there was approval, is that right?
Yeah, that's right. So same idea, if you're willing to do something, and it may not work out and you lose it, you know, you can start all these steps already before you have approval.
With this method of creating a vaccine, are there any safety concerns that people should have, compared to the way a normal vaccine is developed?
No. The regular safety assessments, the processes that are laid out by the regulators that are required for approval, are all the same.
You still saw that all these candidates went through Phase One, Phase Two studies and Phase Three studies and that the results have to be reported and reviewed by Health Canada.
In the case of the clinical trials, you remember, there was here and there a case where an individual had come down with disease and then needed to be specifically reviewed by the review board. The processes are the same as we would normally do for any vaccine.
Will there be any lasting impacts in our development of vaccines after this? Or was this a one-off, and you're not going to see this kind of cooperation again for future vaccines?
Well, I think we're seeing a shift in the field. I think we will see in the future that the times of developing vaccines in 10 to 15 years are over and vaccines will be developed much faster.
Whether it's always as fast as this one, I can’t see that happening, because the money that has gone into this, of course is enormous, right?
In the situation of a global pandemic, yes, I can see that. But if it's a regular disease, which maybe doesn't have the global impact, it's hard to imagine that there will be billions of dollars coming from every government in the world towards the development of these vaccines.
What is the status of your work on a COVID-19 vaccine?
We're making what is called a protein subunit. This is a proven technology that is in a number of vaccines for humans. Diphtheria, tetanus, and whooping cough vaccines for children or the Hepatitis C vaccine.
VIDO-InterVac is making a protein subunit vaccine which also has a lot of advantages in that it's easy to manufacture, it's cost effective and much easier in terms of storage.
The Pfizer vaccine, for example, requires -70 C storage and so on. Our technology does not require that.
We have now made an application to Health Canada - in fact, it's going out today - an official package, which shows all the data that we have on our vaccine candidate and the regulators will review that data and then hopefully give us permission to start our clinical trials in the very near future.
So we're ready to go and waiting now for the green light from Health Canada to start.
In a best case scenario, when might your vaccine be in use in the general population?
It will be later next year at the earliest. I think for most of the vaccines that we're seeing right now, probably around May or June of next year, somewhere there, so ours will be a little bit later than that.